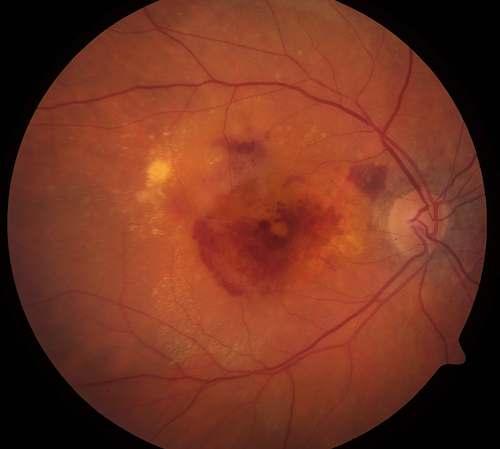 
Telephone calls were performed twice in the first year of randomization and annually thereafter to collect information about adverse events as well as treatment for AMD and incidence of cataract surgery between the study visits. Questionnaires administered at the baseline and annual study visits were used to collect information on nutrition, medications, adverse events, and treatment compliance, among others. In this study we used the recently recommended and more inclusive definition of “late AMD”, which includes any definite GA in the definition, not just central GA. In AREDS2, late AMD was defined as having at least 2 features of neovascularization including serous detachment of the sensory retina, hemorrhage, retinal pigment epithelial detachment, fibrous tissue, or hard exudates or geographic atrophy of an area of 360 μm or greater in diameter, involving the center of the macula or a history of treatment for neovascular AMD. The main study outcome is the development of late AMD as graded from annual fundus photographs. 
These images were assessed by trained graders using a standardized protocol at the University of Wisconsin Fundus Photograph Reading Center. At the baseline and each annual study visits, comprehensive eye exams were performed, including stereoscopic fundus photographs by certified photographers. The AREDS2 participants were randomly assigned to placebo, lutein/zeaxanthin, docosahexaenoic acid (DHA) plus eicosapentaenoic acid (EPA) or the combination. Institutional review board approval was obtained at each clinical site, and written informed consents for the research were obtained from all study participants. At enrollment, participants were included if they had either bilateral large drusen or unilateral late AMD in one eye and large drusen in the fellow eye. 39 Betwparticipants ranging from 50 to 85 years of age were enrolled at 82 retinal specialty clinics in the United States. The study design for AREDS2 is detailed in a previous report but briefly summarized here. 39 These participants were followed for a median of 5 years and the observational data from this study provided the opportunity to investigate the effect of statins on progression to late AMD. The Age-Related Eye Disease Study 2 (AREDS2) was a prospective, multi-centered clinical trial that tested oral supplements of omega-3 fatty acids and lutein/zeaxanthin for the treatment of AMD and cataract. 
34– 37 Lipid lowering with 40 mg of simvastatin in a small proof of concept study, was associated with a possible beneficial effect especially for those persons with bilateral intermediate AMD and those with genotype of the risk alleles for Complement Factor H (CFH) for progression to late AMD. Previous observational studies demonstrated that statin use was associated with a protective effect on AMD 24– 33 however, other studies were not confirmatory. 17– 20 Pathological studies in AMD have also demonstrated the accumulation of lipids in Bruch’s membrane similar to the atherosclerotic changes of cardiovascular disease 21– 23, suggesting that statins might have an effect on AMD. 16 However, this class of drugs has exhibited unexpected anti-inflammatory, antioxidative, and anti-angiogenic effects. 15 The main role of statins is to inhibit 3-hydroxy-3-methyl-glutaryl-CoA reductase in the liver, down-regulating lipid metabolism. Statins, or 3-hydroxy-3-methylglutaryl-coenzyme A reductase inhibitors, currently the most commonly prescribed lipid-lowering class of drugs, 14 are proven to lower serum lipids and reduce cardiovascular morbidity and mortality. 7– 11 This potential inflammatory pathway is further supported by the statistically significant association of elevated serum C-Reactive Protein (CRP) with AMD in the Women’s Health Study, Rotterdam Study, and AREDS. 6 The association of genetic polymorphism in the complement pathway involving complement factor H and many other complement factors suggest that local or systemic inflammatory pathways may also be important in the pathogenesis of AMD. The use of antioxidant vitamins and minerals, known as the Age-Related Eye Disease Study (AREDS) supplement, reduces the risk of progression to late AMD, suggesting that oxidative stress may play a role in AMD. Associated risk factors include increasing age, cigarette smoking, hypertension, increased body mass index, lower educational level, presence of lens opacities, and others 2– 5. Age-related macular degeneration (AMD), a progressive disease that results in central vision loss, is the leading cause of blindness in persons over the age of 60 years in the United States.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
